Achieving people-centred, integrated care through place-based learning: a systems-based approach to learning, developing and improving
By Ruth Germaine, NIHR Applied Research Collaboration Kent, Surrey and Sussex (ARC KSS) Organisation and Research Capacity (ORCA) Strategy Group member. Ruth is also Kent and Medway’s Strategic Lead for Advancing Practice and Independent Prescribing based at Kent and Medway Clinical Commissioning Group.
Whilst there is a global and national drive to achieve people-centred, integrated health and care there is limited discussion about how to develop the workforce required to achieve and sustain this transformation.
Aiming to embed cultures of lifelong learning, improving and innovation through workforce development to transform the workforce and care delivery across its 17 Primary Care Networks (PCN) the East Kent Training Hub considered place-based learning (PBL) as a potential enabler of change to achieve their ambition. As a Darzi Fellow I was asked to consider what was PBL and what needed to happen to embed this in practice.
A previously undefined term with minimal reference within the health and social care literature I - together with the project team - brought together all PCN stakeholders to co-create a deeper understanding of PBL inviting people to attend workshops to share their values and insights. What emerged, along with enablers and outcomes, were three defining values of PBL and three key enablers to embed this in practice.
People-centred learning
Central to PBL, people-centred learning embraces our people and the people in our communities, understanding their wider social context. Built upon compassionate and respectful relationships that embrace the uniqueness and attributes of all people, people-centred learning adapts and responds to different stages and styles of learning and realises the interdependence between what is learnt with outcomes that focus upon what matters to people. Seeing everyone as an asset to be engaged with and inform learning is a win-win for all, increasing happiness, joy, and improved pathways for care that work for all people.
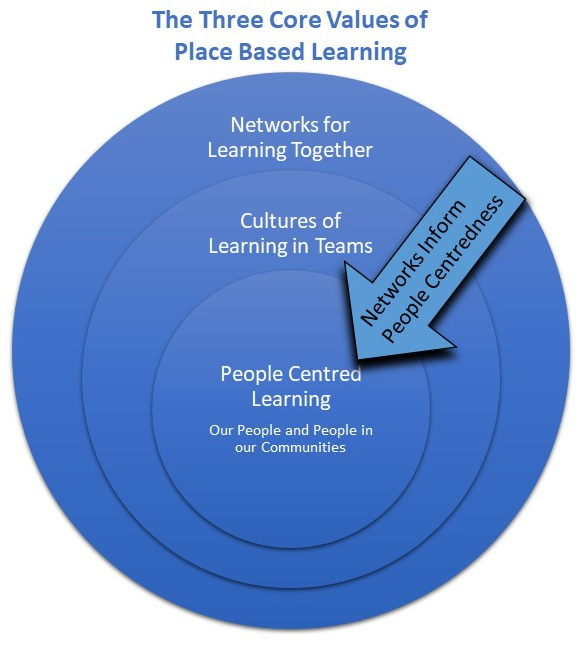
Cultures of learning in teams
Team culture directly impacts both behaviours and outcomes. Embracing people-centred learning at its core cultures of learning in teams are built upon trust creating supportive, open, honest environments where people are nurtured, given time to enquire, innovate and try out new things with the right to fail, celebrate success, reflect, and learn. Valuing learning, enquiring, and improving cultures of learning in teams directly impacts personal development, embedding of knowledge into practice and drives professional, safe effective care and sustainable transformation across the system.
Networks for learning together
Embracing the first two values of PBL networks for learning together extend beyond teams and their organisations to the wider system of health and care, education and people in our communities and the social contexts of which they are a part. Developing collaborative networks builds learning systems that understand, flex, and respond to people’s unique needs and what matters to them whilst building community flouring, improving population health, and reducing health inequalities.
It is these networks for learning together that differentiate place-based learning from work-place Learning which embrace the first two values. Inclusive, enquiring, listening networks for learning and co-creating together inform people-centredness and people centred learning. To achieve the global and national ambition of integrated people-centred care, understanding what is happening, what matters to people and how to help them achieve this in ways that work for them, our people and communities through networks of learning together is pivotal.
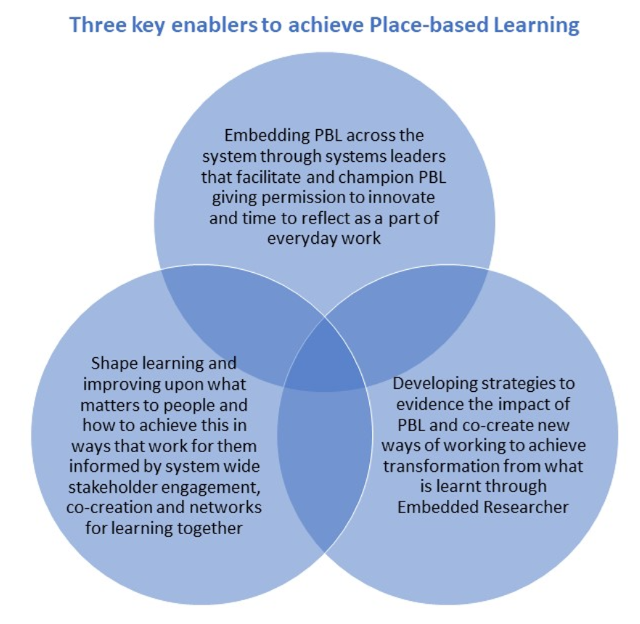
Key enablers of place-based learning
There were many enablers that emerged from the co-creation workshops however, there were three key enablers that were considered pivotal to embed PBL in practice seen below.
The East Kent Training Hub has funded community education facilitators within each of its 17 primary care networks to act as leaders and champions to facilitate PBL in practice, an innovation that has now spread across Kent, Surrey and Sussex. However, for PBL and its potential to be achieved there needs to be a system wide approach to embed this in practice across integrated care systems.
This blog references, is based and reflects upon the full article by Ruth Germaine, Kim Manley, Kim Stillman and Peter J. Nicholls which can be found here IDPJ_12_01_04.pdf (fons.org)








